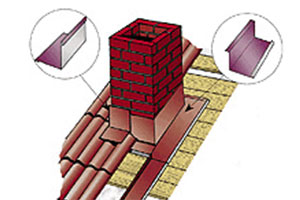
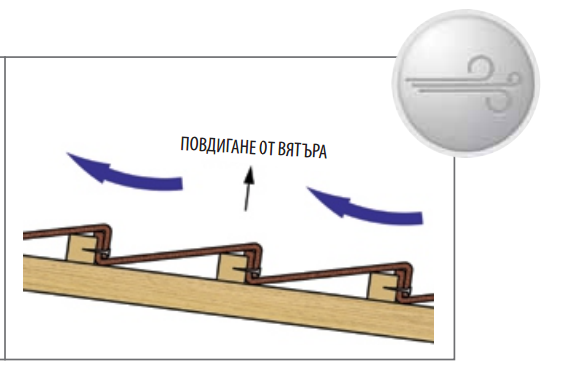
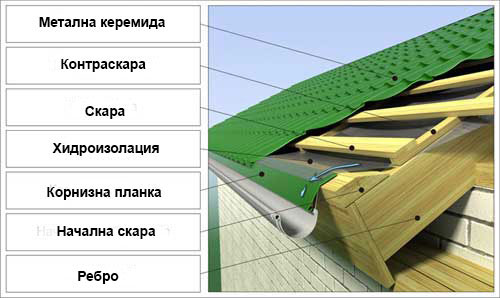
Метални керемиди BILKA Iberic Grande Mat | МЕТАЛНИ КЕРЕМИДИ | Център за покривни материали, София - ROOFER

Монтаж на метални керемиди. | Доставка и монтаж на Метални керемиди и аксесоари. Тел 0896 433 089 ☎️ Email danistroi-90@abv.bg 📧 | By Ново Строителство и Довършителни ремонти.0896433089" am-pokrivi.com | Facebook